When it comes to quality-of-life issues for people with cancer and survivors, the phrase “side effects” comes to mind first. The oddly neutral term comprises the numerous and serious ways that cancer treatment can adversely affect one’s life—during treatment and often for months or even years afterward. Traditional cancer treatments can be notoriously difficult—they’re called “slash, burn and poison” for a reason. And side effects from newer targeted therapy and immunotherapy drugs can range from mild to, on rare occasions, life-threatening.
One of the more difficult side effects that can accompany therapy and persist for up to a decade afterward is cancer-related fatigue. “It affects up to 90 percent of cancer survivors, and it’s a form of fatigue that cannot be alleviated by rest or sleep,” says nutritionist Julia E. Inglis, RD, PhD, of the University of Rochester Medical Center in New York. “It just continues to debilitate people and really affect their quality of life.”
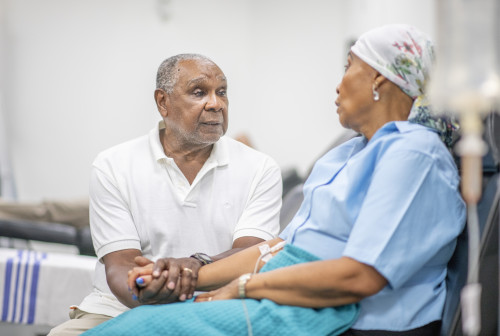
Istock (Model(s) used for illustrative purposes only)
Such a serious, life-altering and nearly universal problem for people with cancer should certainly be the subject of intensive research, right? Wrong. In a recent study, Inglis and colleagues found that despite the changes in appetite, metabolism and body composition that patients with fatigue may experience and despite the importance of good nutrition before, during and after cancer treatment, almost no research has been done on nutritional interventions for fatigue. “This is a neglected area of research,” Inglis says.
Anxiety is another nearly universal side effect of the cancer experience. In one study, funded by the patient advocacy organization Kidney Cancer Research Alliance (KCCure), anxiety and lack of confidence in the cancer care system ranked high as a common side effect among the 450 patients surveyed. “We’ve also looked at the type of follow-up care patients get, and we think the fact that it’s not standardized contributes to this distrust patients feel,” says KCCure founder and president Dena Battle. She’d like to see accepted standards for patients and “a lot more non-industry-funded clinical trials that aren’t necessarily geared toward a new therapy but might take a current therapy and manage it better.” (A related mental health issue, depression, affects nearly a quarter of people with cancer.)
In a Food and Drug Administration report on patient experiences with breast cancer treatment—part of an innovative program called Patient-Focused Drug Development—chemotherapy was one of the most frequently mentioned treatments. Many participants described feeling the debilitating side effects of their chemotherapy even years after their treatment ended. “While I read and was told about all the possible side effects, nothing could prepare me for the emotional and mental upheaval I would experience,” one woman in the report recalled. “I literally felt like I was dying, and I questioned my decision to do the chemotherapy. Every day I contemplated quitting.”
A 34-year-old woman, also quoted in the report, reflected on her decision to skip post-chemotherapy adjuvant treatment with aromatase inhibitors, which are prescribed to help prevent recurrence. “My quality of life is more important to me than living with something that makes me feel less like a woman.... I lost the ability to want to be intimate or sexual with anyone, and that’s something that’s very important to me.”

Istock (Model(s) used for illustrative purposes only)
Bearing the burdens of side effects is hard enough. But it becomes even harder when you are also facing another tremendously common challenge for people with cancer, survivors, caregivers and their families: severe financial hardship.
Next: Financial Toxicity.
Read the whole special report...
Side Effects
Drugs That Don’t Make Life Better
The Promise of Patient-Centered Research







Comments
Comments